What is Dermatitis?
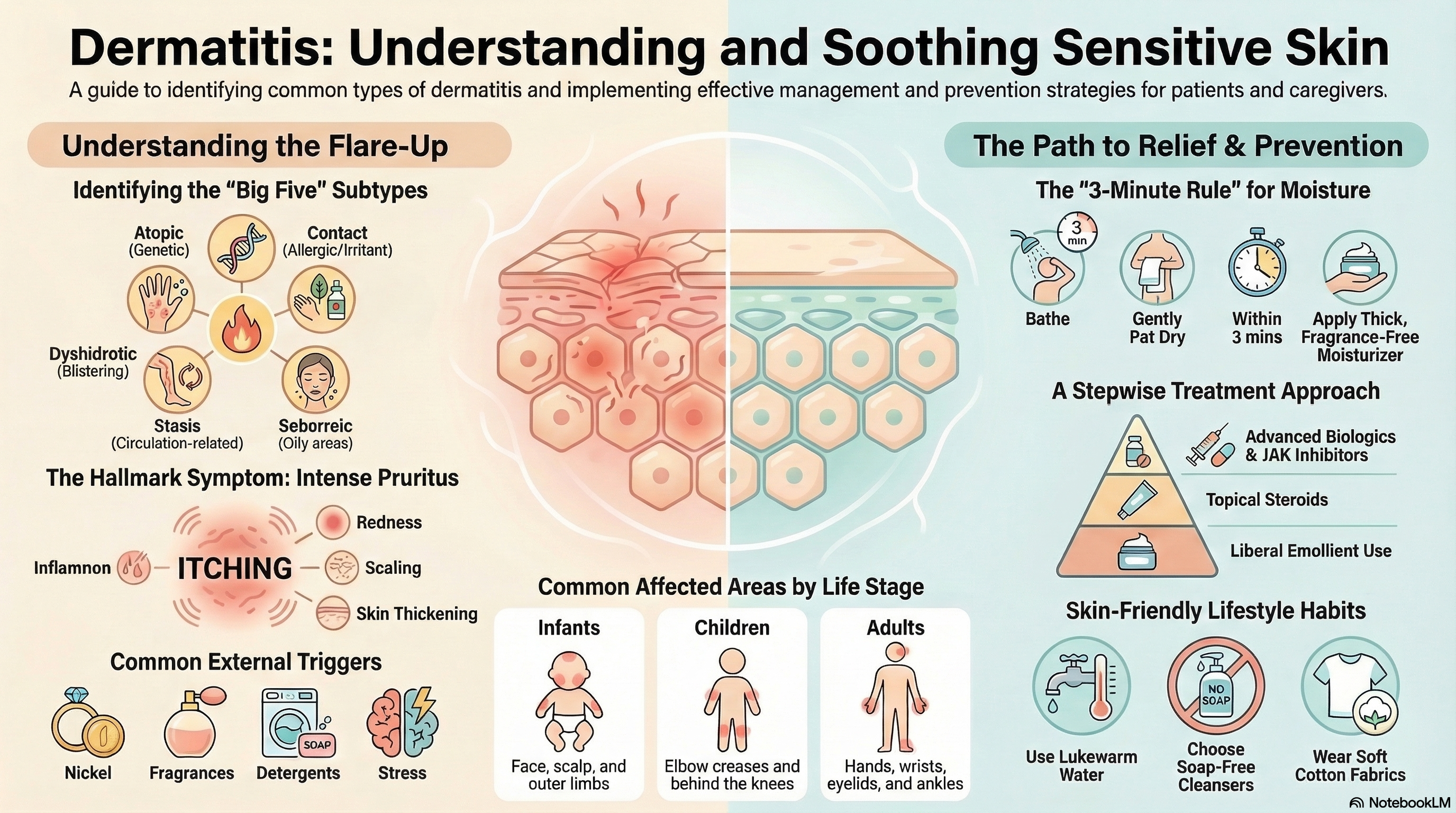
Because "dermatitis" covers so many conditions, it is often categorized by its appearance and where it shows up on the body. The most common subtypes include:
-
Atopic Dermatitis (Eczema): A chronic, relapsing condition driven by genetics and an overactive immune system.
-
Contact Dermatitis: A rash caused by touching a specific substance. This can be allergic (like a reaction to nickel or poison ivy) or irritant (damage from harsh soaps or chemicals).
-
Seborrheic Dermatitis: Known as "cradle cap" in infants or dandruff in adults, this affects oily areas like the scalp, face, and chest.
-
Stasis Dermatitis: Skin changes in the lower legs caused by poor blood circulation and "leaky" veins.
-
Dyshidrotic Eczema: Characterized by tiny, itchy, "tapioca-like" blisters on the palms, fingers, and soles of the feet.
Causes of Dermatitis
The cause varies by type, but most dermatitis involves a breakdown of the skin's natural barrier.
-
Genetics: Many people with atopic dermatitis have a mutation in the filaggrin gene, which helps the skin maintain its moisture barrier.
-
Immune System Overreaction: In many cases, the body's immune system over-responds to small triggers, releasing proteins (cytokines) like interleukin-4 and 13 that cause intense itching and redness.
-
External Triggers: * Allergens: Nickel, fragrances, preservatives (in wet wipes or cosmetics), and topical antibiotics (Neomycin).
-
Irritants: Frequent hand washing, detergents, bleach, and even saliva or urine.
-
-
Microbiome Changes: An overgrowth of certain bacteria, specifically Staphylococcus aureus, can worsen skin inflammation.
-
Environmental Factors: Stress, sweat, cold/dry weather, and rough fabrics like wool.
Symptoms of Dermatitis
While each type has unique features, the hallmark symptoms across almost all forms include:
-
Intense Itching (Pruritus): This is the most common and distressing symptom.
-
Redness and Swelling: The skin may appear red, purple, or brown depending on your skin tone.
-
Dry, Scaly Skin: The skin often feels rough and may flake off.
-
Blisters and Oozing: In acute phases, the skin may develop small bumps that leak fluid and form crusts.
-
Thickened Skin (Lichenification): Over time, constant scratching causes the skin to become thick and leathery.
Location Clues:
-
Infants: Typically the face, scalp, and outer arms/legs.
-
Children: The creases of the elbows and behind the knees.
-
Adults: Hands, wrists, eyelids, and ankles.
Diagnosis of Dermatitis
Diagnosis is primarily clinical, meaning a healthcare provider can usually identify the type of dermatitis by looking at the rash and asking about your history.
-
Physical Exam: The doctor will look at the pattern and location of the rash.
-
History: You may be asked about a family history of the "atopic march" (asthma, hay fever, and food allergies).
-
Patch Testing: If a contact allergy is suspected, a doctor may apply small patches of different substances to your back to see if a reaction occurs after 48 hours.
-
Skin Biopsy: In rare cases where the diagnosis is unclear, a small sample of skin may be taken for lab testing to rule out other conditions like psoriasis or fungal infections.
Treatment of Dermatitis
Treatment follows a stepwise approach designed to calm the current flare and prevent the next one.
-
Maintenance Care: Liberal use of emollients (thick, fragrance-free moisturizers) is the foundation of treatment to repair the skin barrier.
-
Topical Steroids: These are the first-line treatment for active flare-ups. They range from mild (hydrocortisone) to "super-potent" (clobetasol).
-
Non-Steroidal Topicals: Calcineurin inhibitors (tacrolimus) or newer agents like roflumilast and ruxolitinib provide relief without the side effects of long-term steroid use.
-
Biologics: For moderate-to-severe eczema, injectable medications like dupilumab target the specific immune pathways that cause the rash.
-
JAK Inhibitors: A new class of oral and topical medications that provide the fastest relief for intense itching.
-
Phototherapy: Controlled exposure to narrow-band UV light can help chronic, widespread cases.
Prevention of Dermatitis
Preventing flares requires a consistent "skin-friendly" lifestyle.
-
Lukewarm Showers: Avoid hot water, which strips natural oils from the skin. Keep showers short (under 10 minutes).
-
The "3-Minute Rule": Apply a thick moisturizer within three minutes of patting your skin dry after a bath to lock in moisture.
-
Gentle Products: Use only "fragrance-free" and "soap-free" cleansers. Avoid products labeled "unscented," as these may still contain masking fragrances.
-
Soft Clothing: Wear cotton or smooth fabrics. Avoid wool and scratchy synthetics that can trigger itching.
-
Manage Triggers: Use a humidifier in the winter, rinse off sweat immediately after exercise, and keep fingernails short to prevent skin damage from scratching.




