What is Croup?
Croup is an upper airway obstruction that primarily affects children between 6 months and 3 years of age, with the highest incidence occurring in the second year of life. Boys are affected slightly more often than girls (a ratio of 1.4 to 1).
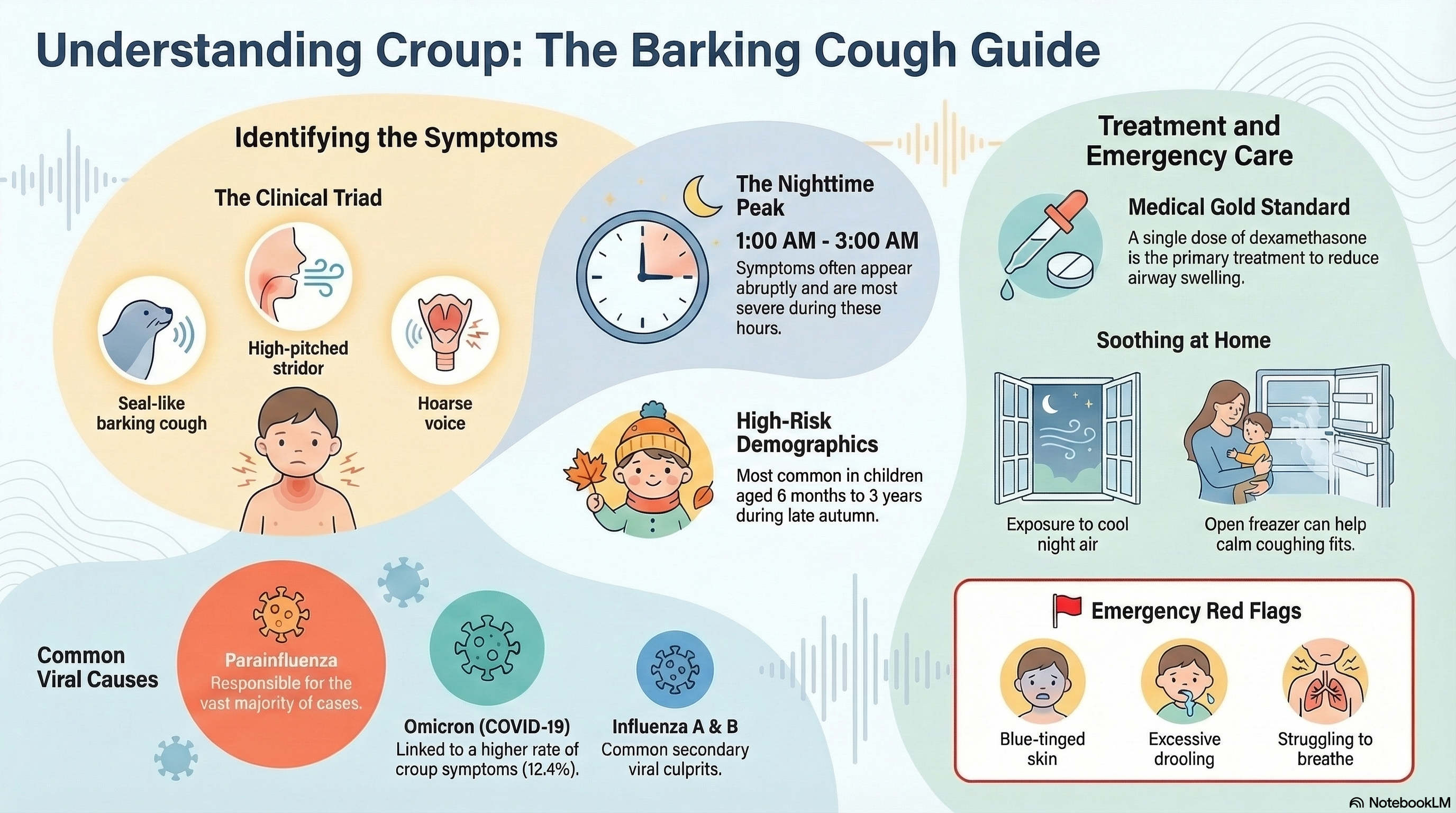
The condition is most common in late autumn (September to December) in North America. It is characterized by a "triad" of symptoms:
-
A barking, seal-like cough.
-
Inspiratory stridor (a high-pitched whistling sound when breathing in).
-
A hoarse voice or cry.
Causes of Croup
Croup is almost always caused by a viral infection.
-
Common Viruses: Parainfluenza viruses (types 1, 2, and 3) are responsible for the vast majority of cases. Other culprits include RSV, influenza A and B, adenovirus, and rhinovirus.
-
COVID-19 Connection: The Omicron variant of SARS-CoV-2 has emerged as a significant cause of croup, with studies showing a higher rate of croup symptoms (12.4%) compared to earlier variants.
-
Environmental Factors: Symptoms often worsen at night, which may be related to natural fluctuations in the body's cortisol levels.
-
Airway Anatomy: Because children have smaller, narrower airways than adults, even a small amount of swelling can cause significant breathing sounds.
Symptoms of Croup
Symptoms typically appear abruptly and are most severe at night, often waking a child between 1:00 AM and 3:00 AM.
-
The Viral Start: Children usually have 12 to 48 hours of typical cold symptoms (runny nose, congestion, low-grade fever) before the barking cough begins.
-
The Barky Cough: This is the hallmark symptom. It is a harsh, brassy cough that sounds like a seal barking.
-
Stridor: A high-pitched, noisy sound heard when the child breathes in. In mild cases, this may only happen when the child is crying or active; in severe cases, it is heard while the child is resting.
-
Respiratory Distress: You may notice "retractions," where the skin pulls in around the ribs or the base of the neck as the child struggles to pull air past the swelling.
Emergency "Red Flags": Seek emergency medical care immediately if your child:
-
Struggles to breathe or has a chest that appears to "cave in."
-
Has blue-tinged lips or skin (cyanosis).
-
Is drooling or has significant difficulty swallowing (this can signal a more dangerous condition called epiglottitis).
-
Is extremely lethargic or difficult to wake up.
Diagnosis of Croup
Diagnosis is primarily clinical, meaning a doctor can usually identify croup just by hearing the characteristic cough and observing the child's breathing.
-
Physical Exam: The doctor will check for stridor and retractions to determine the severity (Mild, Moderate, or Severe).
-
Radiography: X-rays are not usually necessary. However, in atypical cases, a neck X-ray might show the "steeple sign"—a narrowing of the trachea that looks like a church steeple.
-
What is NOT needed: Viral cultures and rapid tests are rarely used because they do not change the immediate treatment plan. If a child appears very toxic, drools excessively, or has a high fever, the doctor will look for alternative diagnoses like bacterial tracheitis or an abscess.
Treatment of Croup
The goal of treatment is to reduce airway swelling and ensure the child can breathe comfortably.
-
Corticosteroids: A single dose of dexamethasone is the gold standard for all children with croup, even those with mild symptoms. It reduces swelling, decreases the need for hospital stays, and usually starts working within 30 to 60 minutes.
-
Nebulized Epinephrine: For moderate to severe cases where the child has stridor at rest, doctors use a "breathing treatment" of epinephrine. This provides rapid relief (within 10 to 30 minutes) by shrinking the swelling in the airway. Children receiving this must be monitored for at least 2 hours to ensure the swelling doesn't return (rebound).
-
Home Comfort: For mild cases, taking the child into the cool night air or sitting in front of an open freezer can often soothe the airway and stop a coughing fit.
-
Hydration: Ensure the child drinks plenty of fluids and use fever reducers (like acetaminophen) to keep them comfortable.
Note: Cough syrups, decongestants, and antibiotics are not effective for croup and should be avoided.
Prevention of Croup
While it is difficult to prevent the common cold viruses that lead to croup, you can reduce the risk and severity of episodes.
-
Hand Hygiene: Frequent handwashing is the best way to prevent the spread of the parainfluenza and respiratory viruses that cause croup.
-
Vaccinations: Staying up-to-date with annual flu shots and COVID-19 vaccinations can prevent some of the viruses known to trigger croup.
-
Avoid Irritants: Exposure to tobacco smoke can irritate a child's airway and may make respiratory symptoms more severe.
-
Monitor Recurrence: If a child has "recurrent croup" (two or more episodes per year), speak with a specialist to rule out underlying issues like allergies or structural airway abnormalities.
Most children recover from the barking cough within 48 hours, though a mild post-viral cough may linger for a week.





